- Drug Topics August 2021
- Volume 165
- Issue 8
OTC and Prescription Products Can Relieve Psoriasis
Pharmacists can educate patients on psoriasis treatments and lifestyle modifications, address expected drug-related adverse effects (AEs), and improve medication adherence.
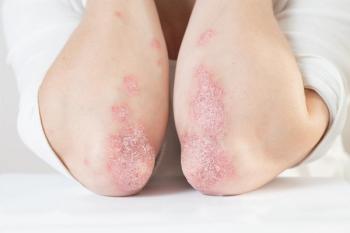
More than 7.5 million individuals in the United States have psoriasis, according to the National Psoriasis Foundation (NPF).1 Psoriasis is a chronic, inflammatory autoimmune disease characterized by raised, red, scaly patches. The majority of patients with mild to moderate psoriasis can control symptoms with topical medications. However, individuals with moderate to severe psoriasis likely will require systemic medications and biologics. Pharmacists can educate patients on treatments and lifestyle modifications, address expected drug-related adverse effects (AEs), and improve medication adherence.
Nonprescription Treatment Options
OTC Products
The NPF and the American Academy of Dermatology have issued joint guidelines for managing psoriasis.2 OTC products are effective for mild psoriasis, and ingredients such as coal tar and hydrocortisone are commonly included.2-4 Pharmacists can recommend products that have the NPF Seal of Recognition, which means they have proven to be nonirritating and safe.4 Coal tar is available in shampoos, creams, ointments, and bath solutions. It works by decreasing itching and flaking; reducing redness, swelling, and scaling; and slowing rapidly growing skin cells.3,4 Hydrocortisone creams and ointments reduce itching and inflammation. If patients have cracked or bleeding skin, hydrocortisone ointments may feel better than creams and cause less irritation.3 Moisturizer helps seal water in the skin to relieve dryness. When selecting a moisturizer, look for a fragrance-free heavy cream, ointment, or oil.3 Patients should apply moisturizer within 3 minutes of bathing and after washing their hands.3 Scale softeners or scale lifters containing salicylic acid remove and soften scales and reduce swelling; they are commonly used to manage scalp psoriasis.4 Ingredients commonly found in scale lifters include lactic acid, urea, and phenol.4
Lifestyle Modifications
Lifestyle modifications can reduce psoriasis flares, reduce the number of medications, and enhance the efficacy of treatments.5,6 Taking daily lukewarm baths with colloidal oatmeal and Epsom salts can help remove scales.5 Pharmacists should educate smokers on the importance of quitting for health benefits and to prevent psoriasis flares.6 Patients should also limit alcohol consumption because alcohol can decrease the efficacy of treatments.5,6 Maintaining a healthy diet and exercising can reduce the risk of developing diseases linked to psoriasis such as diabetes.6
Prescription Treatment Options
Topical Therapies Topical medications are the most common treatments for mild to moderate psoriasis and are typically used as adjunctive therapies for patients taking systemic or biologic agents. Topical corticosteroids are classified into 7 classes that range in strength from ultrahigh (class 1: clobetasol propionate 0.05%) to low (class 6 and 7: triamcinolone acetonide 0.025%, methylprednisolone acetate 0.25%).2 Topical calcineurin inhibitors such as tacrolimus and pimecrolimus can be used as an o-label treatment for psoriasis, and they are especially useful on thinner skin areas (eg, around the eyes) as steroid-sparing agents for prolonged use (> 4 weeks).2 Calcipotriene and calcitriol are vitamin D analogs that slow skin cell growth. They can also be used in combination with topical corticosteroids.2 Tazarotene is a topical retinoid that is more effective when used in combination with mid- or high-potency topical steroids for 8 to 16 weeks for mild to moderate psoriasis.2
Systemic Nonbiologic Treatments
Systemic medications are used to treat moderate to severe psoriasis. Methotrexate (Trexall; AstraZeneca) is taken weekly by oral administration.7 Apremilast (Otezla; Amgen) is an oral medication that does not require laboratory monitoring.7 Cyclosporine is an immunosuppressant taken orally for severe psoriasis, but it is generally not used long term due to the risk of serious AEs.7 Acitretin (Soriatane; Stiefel) is an oral retinoid that typically takes 3 to 6 months to see the full benefits, and it is less effective than other systemic therapies.7
Biologic Therapies
There are 11 FDA-approved biologics for the treatment of psoriasis:
TNF-α inhibitors
- Etanercept (Enbrel; Amgen)
- Infliximab (Remicade; Janssen Biotech)
- Adalimumab (Humira; AbbVie)
- Certolizumab pegol (Cimzia; UCB)
IL-12/IL-23 inhibitor
- Ustekinumab (Stelara; Janssen Biotech)
IL-17 inhibitors
- Secukinumab (Cosentyx; Novartis)
- Ixekizumab (Taltz; Eli Lilly and Company)
- Brodalumab (Siliq; Valeant Pharmaceuticals)
IL-23 inhibitors
- Guselkumab (Tremfya; Janssen Biotech)
- Tildrakizumab (Ilumya; Sun Pharma)
- Risankizumab (Skyrizi; AbbVie)
Biologic agents are administered by injection or intravenous infusion and can be used as monotherapy or combined with topical or nonbiologic systemic medications for the treatment of moderate to severe psoriasis.8 Response to treatment (positive or negative) with TNF-α inhibitors generally occurs after 12 to 16 weeks of continuous therapy, except for infliximab, which should be assessed after 8 to 10 weeks.8 Patients should be evaluated after 12 weeks of treatment with ustekinumab, IL-17 inhibitors, or IL-23 inhibitors.8 Individuals who have partially responded to biologic therapies may have their doses increased, and other drugs, such as topical corticosteroids, can be added to their regimen.8 There are also novel treatments on the horizon for psoriasis that have completed phase 3 trials. Counseling Pearls Pharmacists play an important role in increasing adherence and monitoring for AE in patients taking psoriasis therapies. It is critical to account for patient preferences and daily routines to promote adherence. Patients who would like to avoid injections can receive oral therapies. The NPF is working to help pass legislature for step therapy reform and to reduce out-of pocket costs for patients, which can improve medication adherence and access to care.11 Patients should be empowered to be educated consumers and question their pharmacist and physician about psoriasis treatments.
Pharmacists can take the following steps to ensure optimal use of these medications:
- Counsel patients to give their treatments time, as biologics take approximately 12 weeks to see the full benefits.
- Provide patients with clear written and verbal directions on how to use the medications. Discuss the expected AEs and how to manage them.
- Conduct follow-up phone calls and visits (in person or through telehealth) to assess for adherence and address patients’ concerns.
- Encourage patients to set medication reminders, which also can improve adherence.
Because coal tar can irritate the skin, it is important to test the product on a small area before applying it to regions affected with psoriasis.3 Patients should use salicylic acid products according to the instructions, as too much can worsen psoriasis.3 Using moisturizers along with anti-itch products can help prevent skin irritation.3 Lower-potency corticosteroids should be used on the face, intertriginous areas, and regions that are susceptible to thinning of the skin (eg, forearms). Tazarotene should not be used during pregnancy, and women of childbearing age should have a negative pregnancy test 2 weeks before starting the medication.2 Folic acid or folinic acid supplementation is recommended in combination with methotrexate to reduce gastrointestinal and hepatic AEs.7 Patients taking cyclosporine should have their renal function checked and monitor their blood pressure at home.7 Acitretin is contraindicated in pregnancy because it can cause fetal harm.7 Biologics can increase the risk of infection, and tuberculosis screening is required before initiating therapy.8 The IL-17 inhibitor brodalumab carries a boxed warning regarding rare cases of suicide that have occurred during treatment; patients with a history of suicidal behavior should not receive this medication.8 Brodalumab is only available through restricted access known as the Siliq Risk Evaluation and Mitigation Strategy program.8
Articles in this issue
over 4 years ago
Expanding Access Takes Telepharmacy to the Next Levelover 4 years ago
Exploring the Efficacy, Safety of Rotavirus Vaccinesover 4 years ago
New Prodrug for ADHD in School-aged Childrenover 4 years ago
Flu Season is Approaching, but Experts Don't Know What to Expectover 4 years ago
How to Tactfully Handle Naloxone Counselingover 4 years ago
FDA Grants Priority Review to Tezepelumab for Severe Asthmaover 4 years ago
2021 Good Neighbor Pharmacy of the Year Finalist SpotlightNewsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.