- Drug Topics August 2021
- Volume 165
- Issue 8
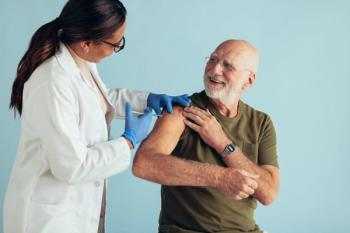
Flu Season is Approaching, but Experts Don't Know What to Expect
Although COVID-19 safety measures helped squash the number of influenza cases last season, pharmacists are revving up vaccination programs and testing.
According to Ann Philbrick, PharmD, FCCP, BCPS, BCACP, an associate professor in the Department of Pharmaceutical Care & Health Systems at the University of Minnesota in Minneapolis, the upcoming season may be “a big question mark.” Because there were so few incidents of the flu last year, it’s “really hard to make recommendations....It’s even possible that the flu vaccines won’t match the flu [strains] very well.”
The CDC reported 2038 flu cases in the United States between September 2020 and April 2021.1 In contrast, approximately 35.5 million individuals were sick with the flu during the 2019-2020 season, which the federal agency describes as “moderate severity.”2
Flu Vaccine Options for the 2021-2022 Season
According to the CDC, health care providers can choose any licensed, age-appropriate vaccine with no preference for any vaccine over another.
For the 2021-2022 flu season, the vaccine options include as follows:
- standard-dose flu shots;
- high-dose shots for individuals aged 65 and older; shots made with adjuvant for individuals aged 65 and older;
- shots made with virus grown in cell culture—eggs are not involved in the vaccine’s production;
- shots made using vaccine production technology— specifically, a recombinant vaccine that doesn’t require having a candidate vaccine virus sample to produce; and
- live attenuated flu vaccine, which is made with attenuated (or weakened) live virus and administered by nasal spray.
Manufacturers estimate that between 194,000,000 and 198,000,000 doses of flu vaccine will be available for the upcoming flu sea- son, according to the CDC. This is more than the 175,000,000 dose record set during the 2019-2020 flu season, the CDC noted.3
Administering Vaccines for COVID-19 and Flu
Jason Mallada, PharmD, BCPS, BCIDP, a clinical pharmacy specialist in infectious diseases and internal medicine at Newton-Wellesley Hospital in Boston, Massachusetts, agreed that it’s almost impossible to predict the rate of flu infections during the upcoming season.
That said, communities are opening up and COVID-19 restrictions are starting to go away, which could mean Americans are at greater risk for both COVID-19 and flu if they’re not vacci- nated, Mallada said. As a result, pharmacists and other health care providers have to be prepared with vaccination programs, in addition to testing for both flu and COVID-19, he said. The CDC’s Advisory Committee on Immunization Practices also recently announced that COVID-19 vaccines can be given to patients at the same time as other vaccines. Health care providers should be mindful of the possibility of increased adverse reactions.4
In May, Reuters reported that COVID-19 vaccine manufacturers are developing and testing booster shots for new variants of the virus; it’s at the discretion of governments around the world as to whether the booster shots are purchased and offered to residents in those countries.5
The news service also reported that the CDC is creating a risk assessment framework to determine the required evidence to recommend a modified vaccine. Both the CDC and other US health agencies are studying ways to assess vac- cine efficiency. Top of mind are the effectiveness of the vaccine among older populations and chil- dren and the impact of new variants.5
The CDC hasn’t officially decided yet whether the US population will need a booster to the COVID-19 vaccine. But Mallada thinks a booster is likely, which means pharmacists need to be prepared to counsel and provide educational materials on COVID-19 and flu vaccines throughout the 2021- 2022 flu season.
In addition, Mallada anticipates increased demand for flu vaccines. To prepare, pharmacies have a sufficient inventory of personal protective equipment and swabs, in addition to vaccines for flu and COVID-19, he said.
Ordering Vaccines and Planning Head
Cleveland Clinic has ordered 2 different flu vaccines for its patients, accord- ing to Allison Riffle, PharmD, associate chief pharmacy officer. One vaccine is for patients aged 6 months to 64 years, whereas the second vaccine is for patients 65 years and older.“ Standardizing in this way was a safety decision. It minimizes errors in helping ensure providers, pharmacists, and caregivers select the appropriate vaccine.”
Riffle added that Cleveland Clinic uses a multidose vial presentation in ambulatory settings, which offers significant cost savings compared with a prefilled syringe. Theresa Tolle, BPharm, FAPhA, owner of Bay State Pharmacy in Sebastian, Florida, plans to start outreach to local employers to educate them about her pharmacy’s test- ing and vaccination capabilities for flu, just as she did for COVID-19 testing and vaccinations. During the upcoming flu season, Tolle expects to recruit retired nurses who can help vaccinate patients and other community members for patient intake, if needed.
Otherwise, she will prepare for the upcoming flu season the same way she has in the past. That includes promoting the flu vaccine through partnerships with senior centers and churches. Tolle started prebooking vaccine orders in January with 5 different suppliers. She plans to have a high-dose flu shot for patients aged 65 and older and a standard-dose shot for her younger customers.
Best Practices for Point-of-Care Testing
Philbrick has 2 best practices for pharmacies that want to provide point-of- care testing for flu:
1. Ensure that there’s a private area for testing in the pharmacy.
2. Assume that the patients who enter the pharmacy for testing are infected; that means patients and pharmacy employees should wear masks and use hand sanitizer.
In addition, pharmacies can participate in collaborative practice agreements, which requires planning, Phil- brick said. These agreements are beneficial for patients who test positive for flu because antivirals, such as oseltamivir (Tamiflu; Roche), which require a prescription, must be taken within 48 hours of the onset of symptoms to be effective.
Alternatively, pharmacies can set up referrals for video-based consults with physicians who can prescribe oseltamivir, according to Philbrick.
Although it’s more work for her employees, Tolle plans to do flu testing on patients in their cars. It takes approximately 20 minutes to get a result, she said. The patient calls the pharmacy from the parking lot, an employee goes out to do the test, and the patient receives the test result.
Florida is a “test-and-treat” state, which means pharmacists can treat patients who test positive for flu with oseltamivir. Pharmacists participating in “test-and-treat” in Florida must complete a 20-hour course approved by the board of pharmacy and carry liability insurance coverage of at least $250,000.6
The future for Pharmacists and Public Health
Tolle points to the role of community pharmacies in West Virginia in bolstering COVID-19 vaccination rates as proof that pharmacists can have a meaningful impact on public health. By January 2021, almost 90% of the state’s vaccine inventory had been used, NPR reported in March. At the same time, some states had only used 30% to 50% of their doses. West Virginia continued to outpace other states that month.7
West Virginia had delivered its vaccine supply to 250 pharmacies; most of the pharmacies were small, independent stores; chain stores such as CVS and Walgreens aren’t common in the state, according to NPR.7
West Virginia was successful because many of its long-term care sites already were partnered with local pharmacies for vaccines and other medicines, in addition to regu- lar COVID-19 testing for residents and staff. The state leveraged those exist- ing partnerships, which helped West Virginia get “an early jump on most other states,” said Krista Capehart, PharmD, BCACP, director of profes- sional and regulatory affairs for the state’s board of pharmacy and chief architect of its COVID-19 vaccination distribution plan, in an interview with NPR.8
“The big picture is that this experi- ence [with COVID-19 vaccines] elevated the importance of pharmacy leaders in primary care in our communities,” Tolle said.“ A leader in a state allowed the independent pharmacists to step up....This is a great case model for how to do [vaccines] well.”
Articles in this issue
almost 5 years ago
Expanding Access Takes Telepharmacy to the Next Levelalmost 5 years ago
Exploring the Efficacy, Safety of Rotavirus Vaccinesalmost 5 years ago
New Prodrug for ADHD in School-aged Childrenalmost 5 years ago
OTC and Prescription Products Can Relieve Psoriasisalmost 5 years ago
How to Tactfully Handle Naloxone Counselingalmost 5 years ago
FDA Grants Priority Review to Tezepelumab for Severe Asthmaalmost 5 years ago
2021 Good Neighbor Pharmacy of the Year Finalist Spotlight