- Drug Topics October 2023
- Volume 167
- Issue 09
The ABCs of CBD: Cannabinoids in Dermatology and Skin Care
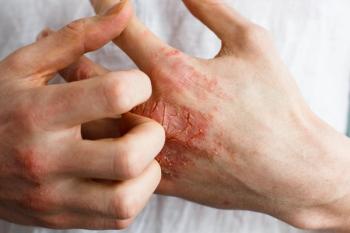
Cannabinoids (CBDs) are gaining popularity in both the skin care industry and the dermatology drug market and are becoming increasingly available to physicians and consumers. Cannabis-based personal care products suddenly seem ubiquitous all over the market, where CBD is a featured ingredient in everything from moisturizers and lotions to makeup.1 In medical dermatology, CBD has been studied in acne, eczematous disorders, lichen planus, melanoma and nonmelanoma skin cancer, melasma, prurigo, pruritus, psoriasis, scleroderma and systemic sclerosis, and seborrheic dermatitis.2
Although some of these studies indicate a potential therapeutic benefit in skin disease, existing studies are, unfortunately, underpowered and lack rigorous design. Making matters worse, the federal government lists cannabis as a Schedule I substance (defined as drugs with no currently accepted medical use and a high potential for abuse), which makes it very difficult to study CBD for medical purposes.
In its last communication on CBD products in the current market, the FDA stated that the existing regulatory framework for CBD is not appropriate and that it will work with Congress to develop a safe and effective regulation strategy. Despite these issues, CBD may offer a promising new area of pharmacology for skin disease and skin care. Even if providers choose not to use or recommend these products, patients are asking about them during their office visits. Therefore, it is important to review the current evidence on CBD use in dermatology to understand its potential for treating skin diseases. It is also important to learn about the potential benefits of CBD in dermatology to better counsel patients in the office.
What Are CBDs?
CBDs are chemicals that exert their effects through cannabinoid receptors (CBRs). Multiple ligands exist for CBRs including endogenous endocannabinoids (such as AEA, 2-AG, PEA, and OEA), phytocannabinoids (produced in plants), and synthetic CBDs. The most notorious and well-known phytocannabinoid is delta-9-tetrahydrocannabinoil (THC), which is the psychoactive component of cannabis responsible for the feelings of euphoria, relaxation, heightened sensory perception, altered perception of time, and increased appetite.
Most CBDs are not psychoactive in the traditional sense. For example, many beauty products contain hempseed oil (cannabis sativa seed oil), which contains no THC. This is an important distinction to make because skin care products labeled “cannabis” can be misleading.
Not only are consumers confused on this topic, but health care providers are as well. A survey of 531 dermatologists found that 64% of respondents did not know that CBD is not psychoactive and 29% did not know that THC is psychoactive.3 Only half of the dermatologists on the Medical Advisory Board for the National Psoriasis Foundation believed that medical cannabis is safe for patients.4
CBRs have been discovered to exist on cutaneous nerve fibers, mast cells, and keratinocytes, and some evidence has shown that CBDs may directly stimulate keratinocytes and act on other important receptors such as PPAR-g (which regulates fatty acid storage and glucose metabolism).5 CBD has also been found to enhance adenosine A2A receptor activity, which downregulates hyperimmune states and decreases tissue inflammation.6
These basic science findings are encouraging and suggest that CBDs may be of benefit in a number of dermatological diseases, as well as for use in personal care products.
“Cannabinoids continue to be of interest as they possess many characteristics that would seemingly make them a great fit for multiple dermatologic conditions: They are potentially anti-inflammatory, anti-pain, and anti-itch; can alter hair growth; can regulate epidermal proliferation; and can even decrease sebum production. In atopic dermatitis, acne, psoriasis, and hidradenitis suppurativa, there is a potential role for them, at least in theory,” said Peter A. Lio, MD, clinical assistant professor of dermatology and pediatrics at Northwestern University Feinberg School of Medicine in Chicago, Illinois, and also the author of the article “Cannabinoids in Dermatology: Hope or Hype?” featured in the Journal of Cannabis and Cannabinoid Research.
CBD and Acne
The pathophysiology of acne is a permutation of follicular hyperkeratinization, microbial colonization, sebum production, and inflammation. The endocannabinoid N-arachidonoylethanolamine glycerol (AEA) has been shown to cause sebocyte apoptosis at higher levels, thus targeting one of the key pathophysiological mechanisms of acne.7 Several in-vitro studies indicate that CBD could be a possible treatment option for acne through its regulatory effects on sebum production and sebocyte proliferation.8
One key study, conducted by Olah et al investigated the effects of CBD on sebaceous glands in vitro.9 The researchers found that AEA (a type of endocannabinoid) was able to inhibit lipogenic actions of sebaceous glands in a dose-dependent manner by inhibiting lipogenic compounds such as arachidonic acid and a mixture of linoleic acid and testosterone. CBD was also found to prevent pro-acne mediators from elevating TNF-a mRNA expression and normalize the lipopolysaccharide-induced expression of IL-1β and IL-6. Furthermore, in a small, split-face study, male subjects applied 3% cannabis seed extract cream to 1 side of their face twice daily for 12 weeks. At the end of the study, researchers found skin sebum production and erythema were significantly decreased compared with placebo, with no notable adverse effects.10
Although larger-scale human studies and randomized, controlled clinical trials are needed in the treatment of acne with CBDs, these preliminary studies show promise in the use of CBD as an individual or adjunctive therapy for acne vulgaris. This may prove popular with patients who are seeking alternative, complementary, or “natural” therapies.
CBD and Atopic Dermatitis/Eczema
CBDs have been studied for the treatment of eczema and atopic dermatitis, which affects about 10% of the US population.11 Eberlein et al studied more than 2000 eczema patients in a large, multinational cohort study and found that applying a cream containing palmitoylethanolamide (PEA) resulted in a significant reduction in dryness, excoriation, pruritus, and erythema across the population. Impressively, 56% of patients stopped using topical corticosteroids by the end of the study.12 It is important to note that this study lacked a placebo group. Therefore, it is difficult to ascertain the therapeutic benefit of the PEA vs the emollient effect of the vehicle. Nevertheless, this study is promising for the use of PEA in the treatment of eczema, as another randomized, double-blind, comparative trial of 60 patients with eczema found that PEA/AEA emollient was associated with improved scaling, dryness, and itching at day 28 of therapy.13
Oral CBD has also been studied for this inflammatory skin disease. Callaway et al found that oral hempseed oil improved AD in a randomized crossover study demonstrating a significant decrease in skin dryness, itchiness, and use of topical medications compared with olive oil.14
CBD: Emollients and Skin Care
CBD has been gaining popularity as a cosmetic material because of its reported emollient and anti-inflammatory properties. Through an examination of online search trends, a 2019 study found that consumer interest greatly increased in topical CBD products from 2015 through 2019.15 CBD has been shown to increase dermal water content and skin turgor.16 CVS.com lists nearly 50 personal care products with CBD, including muscle relief creams, moisturizers, massage oils, facial cleansers, facial masks, antiwrinkle creams, bath salts, and eye serums.17 Sephora.com lists a $125 “full-spectrum CBD” luxury beauty serum, whose description states that “whole plant cannabis molecules penetrate quickly to visibly calm redness, clear blemishes, and deeply restore.”18
Research may support its use here, as well. A mouse model investigating the emollient effect of CBD found that a 1% CBD solution applied to the skin increased the dermal water content through upregulation of aquaporin-3.19 An in vitro study using normal human epidermal keratinocytes found that CBD is able to penetrate keratinocytes and reduce the oxidative stress caused by UVB irradiation and hydrogen peroxide.8
An ideal property of a moisturizer is to treat the pruritus associated with xerosis, and multiple studies have found that anandamide, an endocannabinoid, possesses antipruritic properties via inhibition of TRPV1 (an ion channel expressed mainly in nociceptive neurons of the peripheral nervous system).20
Future Directions
CBD represents an exciting area of pharmacology in the treatment of skin disease and for use in skin care and cosmetics products. CBD has been studied for the treatment of eczematous eruptions, skin cancer, pruritus, fibrotic skin diseases, acne, seborrheic dermatitis, psoriasis, and skin rejuvenation.20 However, most studies are either in vitro studies or clinical studies with only a small number of patients.
Currently, double-blind, randomized, placebo-controlled linical trials for the use of CBD in dermatology are lacking. Preliminary studies show potential benefits but more, well-conducted trials are needed before we can offer definitive recommendations to patients. “It is certainly possible that formulations of cannabinoids can be highly effective, and I remain cautiously optimistic about this. However, that means for now…we are in a tough place and are not really able to recommend cannabinoid products routinely, in my opinion,” Lio concluded.
References
1. Nickles MA, Lio PA. Cannabinoids in dermatology: hope or hype? Cannabis Cannabinoid Res. 2020;5(4):279-282. doi:10.1089/can.2019.0097
2. Mounessa JS, Siegel JA, Dunnick CA, Dellavalle RP. The role of cannabinoids in dermatology. J Am Acad Dermatol. 2017;77(1):188-190. doi:10.1016/j.jaad.2017.02.056
3. Robinson E, Murphy E, Friedman A. Knowledge, attitudes, and perceptions of cannabinoids in the dermatology community. J Drugs Dermatol. 2018;17(12):1273-1278.
4. Nussbaum D, Desai S, Gonzalez-Lopez A, Hawkes JE, Gondo G, Friedman A. Practices and perspectives on medical cannabis and cannabinoids: a survey of the National Psoriasis Foundation Medical Advisory Board. JAAD Int. 2022;9:23-25. doi:10.1016/j.jdin.2022.07.001
5. Gaffal E, Cron M, Glodde N, Tüting T. Anti-inflammatory activity of topical THC in DNFB-mediated mouse allergic contact dermatitis independent of CB1 and CB2 receptors. Allergy. 2013;68(8):994-1000. doi:10.1111/all.12183
6. Burstein S. Cannabidiol (CBD) and its analogs: a review of their effects on inflammation. Bioorg Med Chem. 2015;23(7):1377-1385. doi:10.1016/j.bmc.2015.01.059
7. Dobrosi N, Tóth BI, Nagy G, et al. Endocannabinoids enhance lipid synthesis and apoptosis of human sebocytes via cannabinoid receptor-2-mediated signaling. FASEB J. 2008;22(10):3685-3695. doi:10.1096/fj.07-104877
8. Baswan SM, Klosner AE, Glynn K, et al. Therapeutic potential of cannabidiol (CBD) for skin health and disorders. Clin Cosmet Investig Dermatol. 2020;13:927-942. doi:10.2147/CCID.S286411
9. Oláh A, Tóth BI, Borbíró I, et al. Cannabidiol exerts sebostatic and antiinflammatory effects on human sebocytes. J Clin Invest. 2014;124(9):3713-3724. doi:10.1172/JCI64628
10. Ali A, Akhtar N. The safety and efficacy of 3% cannabis seeds extract cream for reduction of human cheek skin sebum and erythema content. Pak J Pharm Sci. 2015;28(4):1389-1395.
11. Eczema stats. National Eczema Association. Accessed July 9, 2023. https://nationaleczema.org/research/eczema-facts/
12. Eberlein B, Eicke C, Reinhardt HW, Ring J. Adjuvant treatment of atopic eczema: assessment of an emollient containing N-palmitoylethanolamine (ATOPA study). J Eur Acad Dermatol Venereol. 2008;22(1):73-82. doi:10.1111/j.1468-3083.2007.02351.x
13. Yuan C, Wang XM, Guichard A, et al. N-palmitoylethanolamine and N-acetylethanolamine are effective in asteatotic eczema: results of a randomized, double-blind, controlled study in 60 patients. Clin Interv Aging. 2014;9:1163-1169. doi:10.2147/CIA.S65448
14. Callaway J, Schwab U, Harvima I, et al. Efficacy of dietary hempseed oil in patients with atopic dermatitis. J Dermatol Treat. 2005;16(2):87-94. doi:10.1080/09546630510035832
15. Wang JV, Shah S, Albornoz CA, Saedi N. Consumer interest in topical cannabidiol: an examination of online search trends from 2015 to 2019. Clin Dermatol. 2021;39(6):1014-1017. doi:10.1016/j.clindermatol.2020.11.007
16. Palmieri B, Laurino C, Vadalà M. A therapeutic effect of CBD-enriched ointment in inflammatory skin diseases and cutaneous scars. Clin Ter. 2019;170(2):e93-e99. doi:10.7417/CT.2019.2116
17. CBD products. CVS. Accessed July 9, 2023. https://www.cvs.com/shop/personal-care/cbd
18. Saint Jane Beauty Luxury Beauty Serum Calming Treatment. Sephora. Accessed July 9, 2023. https://www.sephora.com/product/luxury-beauty-serum-P444222
19. Ikarashi N, Shiseki M, Yoshida R, et al. Cannabidiol application increases cutaneous aquaporin-3 and exerts a skin moisturizing effect. Pharmaceuticals (Basel). 2021;14(9):879. doi:10.3390/ph14090879
20. Sheriff T, Lin MJ, Dubin D, Khorasani H. The potential role of cannabinoids in dermatology. J Dermatol Treat. 2020;31(8):839-845. doi:10.1080/09546634.2019.1675854
Articles in this issue
over 2 years ago
Preventing Severe Respiratory Infections in Childrenover 2 years ago
Pediatric T1D Management Adherence System Evaluatedover 2 years ago
Sickle Cell Disease Finally Getting Its Dueover 2 years ago
Celebrating Women in Pharmacyover 2 years ago
Biosimilars Are Bringing Affordability and AccessibilityNewsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.