Specialist Care for Shingles Complications
Some patients may benefit from specialized treatment.
The majority of patients diagnosed with
“The main issue with shingles is in patients that are elderly and have more severe cases,” Lindsay C. Strowd, MD, FAAD, associate professor in the Department of Dermatology at Wake Forest School of Medicine told Drug Topics®.
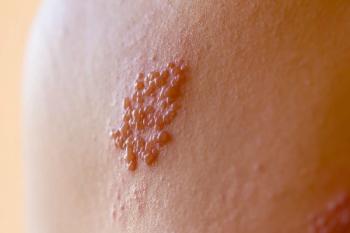
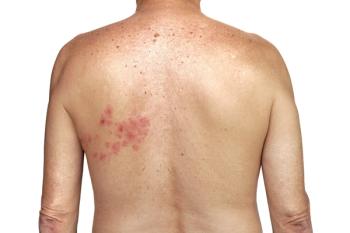
Other high-risk individuals include those receiving chemotherapy or other types of immunosuppressive medications that impair their ability to fight off infections. “They can get a more widespread rash that may not be confined to a local part of the skin,” explains Strowd. “They can get shingles that actually go into their bloodstream or into their cerebral spinal fluid and cause meningitis or other types of more serious infections. It’s one of the reasons that we want to diagnose it quickly and treat it quickly.”
Postherpetic neuralgia (
“In immunosuppressed individuals—for example, people who are on immunosuppressant drugs, people with HIV, people who have an underlying malignancy—shingles can be more severe, and the incidence of postherpetic neuralgia can have a higher frequency,” explains Justin C. McArthur, MBBS, MPH, professor and director of the Department of Neurology, the Johns Hopkins University School of Medicine and past-president of the American Neurological Association.
According to McArthur, prompt treatment of shingles seems to reduce the incidence of PHN and the risk of
“A primary healthcare provider would typically refer the patient to a pain treatment specialist, who might be a neurologist or anesthesiologist. Because these are interventional procedures, they’re usually done in a specialized pain treatment center,” McArthur said.
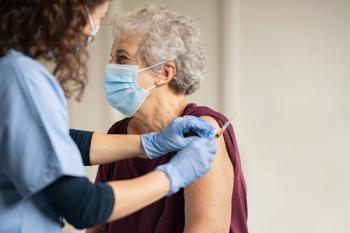
Both McArthur and Strowd recommend vaccination against shingles with
“Even if you do happen to get it again, if you’ve been vaccinated it usually makes the disease course a lot milder and helps mitigate against some of the long-term complications,” Strowd concluded.
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.