Postherpetic Neuralgia Overview
The lowdown on shingles’ most common complication.
Herpes zoster (shingles) is considered to be one of the most
The condition is defined as recurring or persistent long-term nerve pain in an area of the body that has suffered an outbreak of shingles, which is caused by the varicella zoster virus (VZV). The virus initially causes chickenpox in an individual, then goes dormant in their dorsal root ganglia for decades. When it
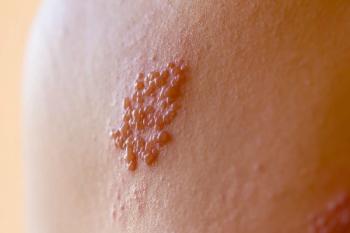
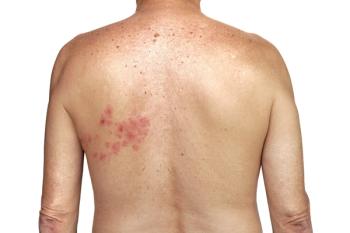
PHN is the result of that nerve damage, and the most common chronic complication of shingles. Its onset typically begins after the shingles blisters crust over and start to heal, but it can also occur in individuals with
Statistics show that approximately 1 out of every 3 people in the United States will develop shingles in their lifetime, or an estimated 1 million cases each year. The
“An older adult with shingles is more likely to develop PHN and have longer lasting and more severe pain than a younger person with shingles. People younger than 40 rarely experience PHN,” according to the CDC.1
DelveInsight's "Postherpetic Neuralgia - Market Insights, Epidemiology, and Market Forecast-2030"
The level of pain associated with PHN is reflected by the types of treatments that are used. It typically requires an individualized, multi-pronged approach using a combination of options.
Transdermal
The only way to avoid both shingles and PHN is through vaccination.
Shingrix has an efficacy rate of over 90% in clinical tests, far surpassing that of the only other shingles vaccine on the market, Zostavax. It also has been shown to induce
References
1. CDC. Shingles (Herpes Zoster). Complications of Shingles. Page last reviewed July 1, 2019. Accessed July 6, 2020.
2. Postherpetic Neuralgia Market Size & Share, Epidemiology and Forecast till 2030. Press Release. DelveInsight. Accessed July 6, 2020.
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.