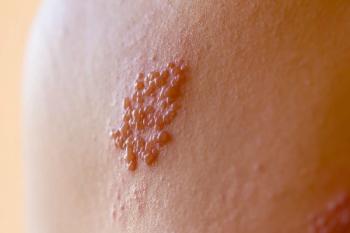
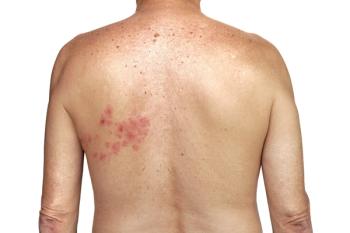
In a discussion of shingles—also known as herpes zoster (HZ)—the focus is generally on the red, blistering rash and nerve pain it causes over a period of weeks. Although HZ is generally self-limiting, potentially serious complications can occur. For up to 4% of patients with HZ, hospitalization is required to treat those complications.1
Older individuals and those who are immunocompromised due to disease or medication are at greater risk of developing serious shingles complications. Approximately 30% of people hospitalized with shingles have compromised or suppressed immune systems.1
According to the CDC, long-term nerve pain called postherpetic neuralgia (PHN) is the most common complication associated with shingles. Confined to the area where the shingles rash occurred, PHN persists for at least 3 months after the rash has resolved. PHN pain can be debilitating and severely curtail everyday activities. Although it can subside over time, PHN can continue for years.
Like shingles, the risk of developing PHN increases with age, with approximately 20% of people aged 70 and older living with long-term pain. 2 Other sensations related to PHN include loss of feeling, tingling, and coldness. Severe cases of PHN can lead to depression, disability, weight loss, and insomnia. Postherpetic itch, another complication, develops in skin with severe sensory loss due to shingles. Scratching the affected area can lead to a bacterial superinfection of the lesions and further injury to the skin. Topical local anesthetics that numb the skin can provide some relief.
Shingles on the face has its own potential for serious complications. Herpes zoster ophthalmicus (HZO), or shingles that occur near or in the eyes, accounts for up to 20% of all shingles cases and is considered a growing problem. Left untreated, up to 70% of patients with HZO develop serious complications that may include sensitivity to light, eyelid swelling, glaucoma, corneal inflammation and scarring, visual impairment, and blindness. Patients who receive a diagnosis of HZO should consult their ophthalmologist immediately for specialized treatment.
Shingles infections that involve the ear—herpes zoster oticus (or Ramsay Hunt syndrome—can cause hearing and balance problems as well as weakness on the affected side of the face that can be long lasting or permanent.
If the varicella-zoster virus that causes shingles spreads to the brain or spinal cord, the potential exists for serious complications like stroke and meningitis, particularly in individuals with HZO.
Regardless of where on the body the shingles rash erupts, it is critical to see a medical professional quickly. Early treatment with antivirals can not only shorten the course of the infection but also help reduce the chance of complications developing.
The CDC’s Advisory Committee on Immunization Practices (ACIP) recommends a proactive approach—getting the recombinant zoster vaccine (Shingrix)—to help prevent shingles and complications from occurring at all. The vaccine is advised for immunocompetent adults 50 years and older and is administered in 2 doses given 2 to 6 months apart.1 It can also be given to individuals who have had a previous case of shingles to prevent a reoccurrence and to those who have had a previous dose of zoster vaccine live (Zostavax), which is no longer available in the United States. More recently, the ACIP unanimously recommended the recombinant zoster vaccine for immunocompromised adults aged 19 and older.2
As noted on the CDC website3: “Shingrix provides strong protection against herpes zoster and PHN. Two doses of Shingrix are more than 90% effective at preventing herpes zoster and PHN. Protection stays above 85% for at least the first 4 years after vaccination.”
References
1. Shingles (herpes zoster). CDC. Updated October 5, 2020. Accessed October 26, 2021. https://www.cdc.gov/shingles/hcp/clinical-overview.html#clinical-features
2. Complications of shingles. CDC. Updated July 1, 2019. Accessed November 2, 2021. https://www.cdc.gov/shingles/about/complications.html
3. Shingles vaccine fact sheet for healthcare providers. CDC. Updated July 1, 2019. Accessed October 26, 2021. https://www.cdc.gov/shingles/multimedia/shingles-factsheet-hcp.html
4. US Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices votes unanimously to recommend Shingrix for immunocompromised adults aged 19 and up. News release. GlaxoSmithKline. October 20, 2021. Accessed October 26, 2021. https://www.gsk.com/en-gb/media/press-releases/votes-unanimously-to-recommend-shingrix-for-immunocompromised-adults-aged-19-and-up/#