Oral Shingles Are A Mouthful of Pain
Prompt treatment can reduce pain and complications.
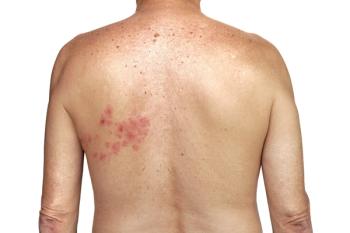
Although not as common as shingles of the skin, oral shingles is associated with singular challenges when it comes to diagnosis and treatment. Like all cases of
Oral shingles presents in
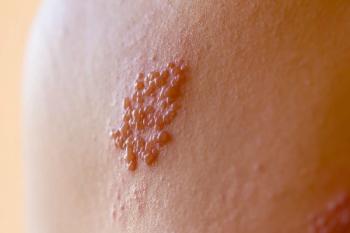
The acute eruptive phase quickly follows and is marked by the eruption of tiny blisters in dense clusters on the mucous membranes of the upper or lower mouth that rapidly become very painful.
“The vesicles rupture pretty quickly in the oral cavity, much faster than they would on the skin because we’re eating and talking, and things are hitting these blisters and rupturing them. When they rupture, they form shallow ulcers and slowly start to phase out,” Sonal S. Shah, DDS, associate professor of oral and maxillofacial pathology and medicine at the University of Nevada, Las Vegas, told Drug Topics®.
Other symptoms associated with the acute eruptive phase include mouth sensitivity, intense pain, loss of appetite, difficulty chewing, and overall body aches.
Shah noted that while oral shingles can be mistaken for other diseases—most commonly, the oral herpes simplex virus (HSV)—there are symptoms that can simplify the diagnosis.
“Cases of true oral shingles tend to be more painful, more diffuse, and require earlier and more aggressive treatment and being on the lookout for postherpetic neuralgia,” she said. “Typically, it’s a clinical diagnosis based on talking to the patient and looking for the unilateral distribution and the nature of the lesions. Oral shingles lesions almost always tend to occur on the palate, or roof of the mouth.”
The chronic, or final, phase of oral shingles is known as postherpetic neuralgia (
Treatment of shingles in general relies heavily on the antiviral drugs valacyclovir, acyclovir, and famciclovir, which are most effective when administered within 72 hours of the onset of symptoms. In cases of oral shingles, there are additional treatments aimed primarily at making the patient comfortable until symptoms clear.
“The mouth is very sensitive, and these patients can really suffer,” said Shah, adding that eating, drinking, brushing, and flossing during an outbreak can be challenging. “Using viscous lidocaine, which is a topical anesthetic, and magic mouthwash, which can have viscous lidocaine and other soothing agents, can certainly help.”
Shah advises patients to wash their hands often to prevent transmission or autoinoculation.
Proper oral hygiene, including the use of chlorhexidine antibacterial mouthwash, is also important to keep the mouth clean, prevent the infection of ruptured blisters, and promote healing.
She also recommends that patients with oral shingles who develop facial postherpetic neuralgia see an oral facial pain specialist for an evaluation and a prescription for a neuropathic medication like gabapentin.
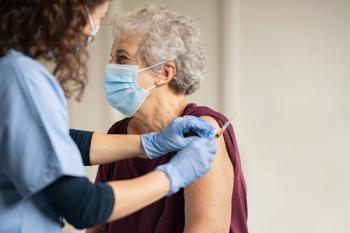
Individuals who have healed from a shingles outbreak should consider getting the recombinant zoster vaccine (
Reference
1. Get the Shingrix vaccine if you are 50 or older. CDC. Updated July 2, 2019. Accessed December 21, 2021.
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.