Recurrent Shingles: Herpes Zoster Can Strike More Than Once
Here’s what to know about recurrent shingles and risk factors.
Individuals who have experienced the painful and often debilitating condition known as shingles (herpes zoster, or HZ) would like to think that it’s a 1-and-done infection. Unfortunately, although a reoccurrence of shingles is not common, it can and does happen due to the innate nature of the varicella zoster virus (
VZV does not discriminate by age. The virus is at the root of both the childhood infection known as chickenpox (varicella) and the adult infection
Once the primary infection (chickenpox) resolves, VZV moves into the dorsal root ganglia where it remains dormant for decades. It can then
According to the
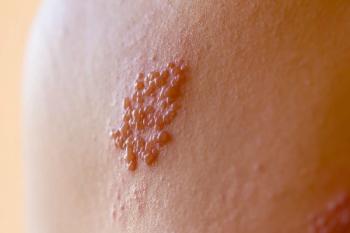
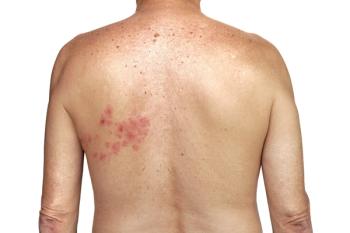
Recurrent shingles — that is, any occurrence of shingles that happens after the initial case — is basically another reactivation of the VZV that’s already in the body. As long as VZV is present, there’s always a chance of relapse and another episode of shingles. Risk factors for recurrent shingles are primarily linked to the overall condition of an individual’s immune system. Immunocompromised people are particularly prone to relapse.1
Other risk factors include age (attributable to weaker immune systems), gender (women account for 60% of all recurrent shingles cases), high anxiety and stress levels, certain immunosuppressive therapies, cancer, autoimmune diseases like HIV/AIDS and lupus, and chronic diseases like diabetes, hypertension, and chronic obstructive pulmonary disease.1
The time period between an initial case of shingles and a reoccurrence can vary, but researchers have identified a 4- to 8-year window as most likely. A
“Our high HZ recurrence rates suggest that zoster vaccination should be offered in people who have had an HZ episode to prevent potential recurrences,” the study’s authors concluded.2
Shingrix, the shingles vaccine that was introduced in the United States in 2017, is the first line of defense against shingles and its complications. As individuals age, their immune systems decline, increasing their risk of developing shingles. Shingrix works by helping the immune system defend against shingles.
Two doses of Shingrix administered 2 to 6 months apart have been proven to be more than 90% effective at preventing HZ and PHN. The vaccine offers continued protection for at least 4 years.
Shingrix is recommended by the CDC’s Advisory Committee on Immunization Practices for use in immunocompetent adults 50 years and older. It can be administered to a patient with shingles once the rash has healed to protect against future reoccurrences and related complications.
References
1. CDC. Shingles (Herpes Zoster). Updated October 5, 2020. Accessed June 30, 2021.
2. Yawn BP, Wollan PC, Kurland MJ, Sauver JL, et al. Herpes zoster recurrences more frequent than previously reported. Mayo Clinic Proceedings. February 2011. doi:10.4065/mcp.2010.0618
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.