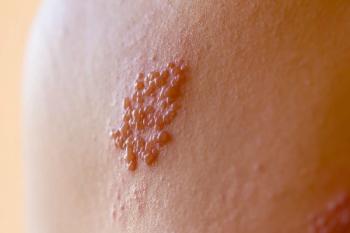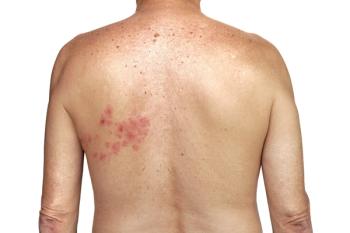
Immunocompromised Patients at Greater Risk for Shingles
Cancer, HIV, and organ transplants can also increase the risk of shingles.
Prompted by that knowledge and the fact that estimates of HZ risk by immunocompromising medical conditions has not been well characterized, investigators at the CDC and Fred Hutch Cancer Research Center at the University of Washington conducted a comprehensive systemic review of medical literature. Their findings were recently published in
The scientists focused on estimated HZ risk in 6 categories of immunocompromised patients: hematopoietic cell transplants,
“HZ is common among all immunocompromised populations studied, exceeding the expected HZ incidence among immunocompetent adults aged ≥ 60 years,” the investigators concluded. They added that better evidence of the incidence of HZ complications and their severity in immunocompromised populations is needed to inform economic and HZ vaccine policies.1
A second separate statistical analysis was conducted at the Faculty of Pharmaceutical Sciences at the University of British Columbia in Canada. Subsequently
The meta-analysis demonstrated that immunosuppression through HIV/AIDS or malignancy significantly increased the risk of HZ compared with controls. Family history, physical trauma, and older age were also shown to be associated with a greater risk. Other risk factors include psychological stress,
“Many of these characteristics are known well in advance by the patient and clinician and may be used to guide discussions with patients for prevention by vaccination,” the investigators concluded.2
The Shingrix vaccine was proven in clinical trials to be over 90% effective in the prevention of shingles, and a recent study concluded that it is
Administered in 2 doses given 2 to 6 months apart, Shingrix helps defend the immune system against the resurgence of the
References
1. Dooling KL, Guo A, Pergam SA, McKay S. 1629. Herpes zoster risk in immunocompromised adults in the United States: A systematic review. Open Forum Infectious Diseases. 2019.
2. Marra F, Parhar K, Vadlamudi N. Risk factors for herpes zoster infecton: A meta-analysis. Open Forum Infectious Diseases. 2020.
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.