- Drug Topics April 2023
- Volume 167
- Issue 04
Safety, Accuracy of Dexcom G7 CGM Evaluated in T1D and T2D
The CGM provides accurate readings over 10.5 days of continuous wear.
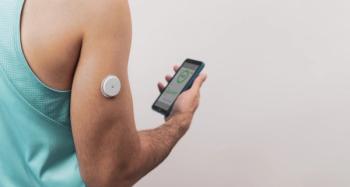
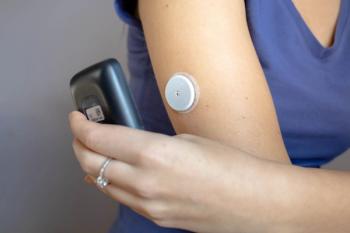
The Dexcom G7 continuous glucose monitor (CGM) can provide accurate glucose readings with either arm or abdominal placement over a period of wear of 10.5 days, according to research published in Diabetes Technology & Therapeutics.1
In a prospective, multicenter, single-arm study (NCT04794478), researchers evaluated the safety and accuracy of the Dexcom G7 CGM in adults with diabetes. Over a 10.5-day wear period, performance of sensors worn on the arm and abdomen were assessed for glucose concentration ranges and rates of glucose changes.
Researchers enrolled 318 adults aged 18 to 78 years with type 1 diabetes (T1D), intensive insulin therapy type 2 diabetes (T2D), or non-intensive insulin therapy T2D; participants also demonstrated a willingness to wear up to 3 Dexcom G7 sensors for the duration of the sensor, as well as to avoid injecting insulin or wearing an insulin pump infusion set within 3 inches of the insertion site.
Participants wore G7 sensors on the back of the upper arm and the abdomen and were told to continue their typical practices to monitor glucose—including blood testing or use of a personal CGM—diabetes management regimens, and other activities. Three 12-hour clinic sessions on days 1 or 2, days 4 or 7, and the second half of 10 day or first half of day 11 of the wear period were scheduled. At these visits, comparisons were made with comparator blood glucose measurements obtained via the YSI 2300 Stat Plus glucose analyzer. Accuracy metrics were evaluated as the proportion of CGM values within 15%, 20%, and 30% of paired YSI values (>100 or 15 mg/dL, 20 mg/dL, or 30 mg/dL of YSI values ≤100 mg/dL, respectively [%15/15, %20/20, and %30/30]).
Within the cohort, mean age was 44.3±15.7 years; 80.8% of patients were diagnosed with T1D, 16% with intensive insulin therapy T2D, and 3.1% with non-intensive therapy T2D. Just over half (53.5%) were women, and 89.9% were white. More than two-thirds of participants were overweight or obese, “consistent with the prevalence of these conditions among people with diabetes in the United States,” according to researchers.
In total, 316 participants provided CGM data from 308 arm and 311 abdominal sensors, representing 79,003 CGM-YSI matched pairs. Among these pairs, 77,774 were in the reportable range of 40 to 400 mg/dL (39,193 arm devices and 38,581 abdominal devices) that were included in the calculation of accuracy.
Overall mean absolute relative difference for arm and abdominal sensors were 8.2% and 9.1%; %15/15, %20/20, and %30/30 agreement rates for each site were 89.6%, 95.3%, and 98.8% (arm) and 85.5%, 93.2%, and 98.1% (abdominal), respectively.
Among the 308 arm sensors, 94.5% had >80% of CGM-YSI matched pairs that met criteria for %20/20 accuracy; among the 311 abdominal sensors, 8.5% met that same criterion. Mean and median per-sensor mean absolute relative differences were 8.8% and 7.8%, respectively.
Per investigators, accuracy was high in both arm- and abdominal-placed sensors over the 10 day-wear period through the 12-hour grace period and across glucose ranges. No statistically significant differences were noted between G7 accuracy when participants were analyzed by type of diabetes and insulin regimen.
No serious adverse events were noted in the study population, although 4 participants noted mild to moderate device related adverse events, including moderate erythema at the insertion site on the arm and adhesive areas, mild skin tearing at the adhesive area on the abdomen, moderate erythema at the adhesive area on the abdomen, and mild and moderate discomfort during sensor removal.
Overall, 75.8% of the cohort had experience with a personal CGM; within this group, 68.1% found the G7 easier to insert compared with their current CGM device. Just over half of participants (51.7%) indicated that they preferred to wear the sensor on the arm.
Study limitations include the exclusion of children and adolescents, as well as the potential lack of generalizability to those who are not White, overweight, or obese. Additionally, the study was not designed to evaluate outcomes including HbA1c reduction.
“This study demonstrates that the G7 CGM is accurate and safe to use for up to 10.5 days in adults with diabetes when worn on either the arm or abdomen,” the researchers concluded. “The enhanced features of G7 may increase clinical adoption, encourage sustained use, and reduce the burden of diabetes management.”
Disclosures: Several study authors reported relevant financial relationships. For the full list, please see the study.
Reference
1. Garg SK, Kipnes M, Castorino K, et al. Accuracy and safety of Dexcom G7 continuous glucose monitoring in adults with diabetes. Diabetes Technol Ther. 2022;24(6):373-380. doi:10.1089/dia.2022.001
Articles in this issue
almost 3 years ago
Case Study: Treating Infants for Cannabis Exposurealmost 3 years ago
Oral Treatment Approved for Anemia Caused by CKDalmost 3 years ago
A Return to Normalcyalmost 3 years ago
Oncology Pharmacists Are Crucial in Skin Cancer Managementalmost 3 years ago
What Pharmacists Need to Know About Point-of-Care Testing for STIsalmost 3 years ago
A Biosimilar Wave Looms Large Over US Biologics Marketalmost 3 years ago
The JAK Inhibitor Pipeline Builds in Dermatologyalmost 3 years ago
Kudos to WHOalmost 3 years ago
How Pharmacists Should Talk So Vaccine-Hesitant Parents ListenNewsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.