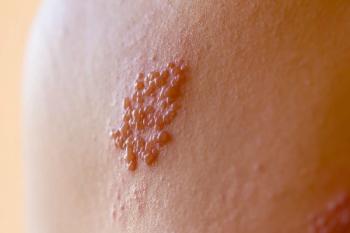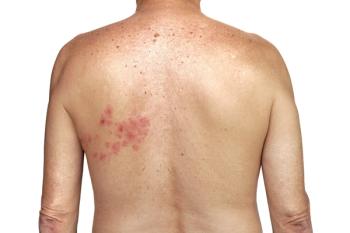
Herpes Zoster Ophthalmicus and Vision Loss
Moderate to severe vision loss occurs in 10% of cases, study says.
Of the estimated 1 million cases reported each year in the United States,
HZO occurs when the dormant
The Australian study focused on determining the rate of moderate and severe vision loss following HZO, and identifying causes and factors associated with permanent vision loss due to HZO.1
Investigators reviewed the records of 869 patients with acute HZO who were seen at 1 center between 2006 and 2016. The median follow-up time was 6.3 years. Ocular involvement occurred in almost 85% of cases. Moderate vision loss, defined as greater than or equal to 20/50, and severe vision loss (≤20/200) secondary to HZO were both measured. Moderate loss occurred in 83 eyes (9.6%), whereas severe vision loss occurred in 31 eyes (3.6%).1
Conjunctivitis, keratitis, and uveitis were the most common sites of ocular involvement. The causes of vision loss included corneal scarring (94%), corneal perforation (4.8%), and secondary glaucoma (1.2%).1
“Among individuals with HZO, approximately 1 in 10 individuals may develop moderate or severe vision loss, primarily due to corneal scarring,” the investigators concluded.1 “Older age, immunosuppression, and uveitis are associated with severe permanent loss of vision secondary to HZO.”
Vaccination is the best available protection against herpes zoster and HZO.
The American Academy of Ophthalmology (AAO) issued a
“Vaccination starting at 50 years of age will reduce the burden of this disease, including chronic eye disease,” the statement concluded.3
AAO encourages ophthalmologists to proactively promote shingles vaccination to their patients by partnering with
References
1. Niederer RL, Meyer JJ, Liu K, Danesh-Meyer HV. Herpes zoster ophthalmicus clinical presentation and risk factors for loss of vision. American Journal of Ophthalmology. February 8, 2021. Doi:
2. Kong CL, Thompson RR, Porco TC, Kim E, Acharya NR. Incidence rate of herpes zoster ophthalmicus: A retrospective cohort study from 1994 through 2018. October 9, 2019. Doi:
3. Recommendations for herpes zoster vaccine for patients 50 years of age and older. Policy statement. American Academy of Ophthalmology; August 17, 2018. Accessed April 29, 2021.
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.