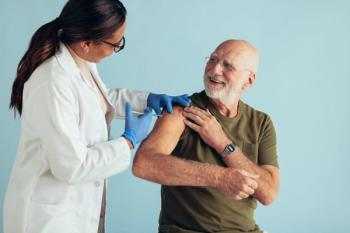
How Pharmacists Can Address Vaccine Hesitancy for the Flu and Beyond
Address vaccine hesitancy at your pharmacy to encourage patients and their families to get vaccinated against COVID-19, flu, and more.
According to the World Health Organization (WHO), vaccine hesitancy is when patients delay their acceptance or refuse safe vaccines despite vaccines being available to them.1 It’s not a new problem, but a July 2022 review article on the subject in the New England Journal of Medicine describes it as a problem that has “escalated in scope and scale.”2
The review noted how easily social media has enabled misinformation and disinformation to spread. “The hyperconnected digital landscape offers a new opportunity for people with shared beliefs to self-organize across geographic regions, influencing and sometimes disrupting public confidence and cooperation,” the authors wrote.2 This combined with the declining trust in experts have resulted in lower vaccine coverage rates. “Equipping physicians with information on the nature and scope of circulating concerns in their communities may help them address such concerns in the clinic, while also informing appropriate interventions at the community level,” the authors concluded.2
Brigid Groves PharmD, MS, senior director of practice and professional affairs at the American Pharmacists Association (APhA) in Washington, DC spoke with Drug Topics® on ways pharmacists combat vaccine hesitancy and increase vaccination rates to protect their patients. She said that in addition to the spread of misinformation and disinformation, socioeconomic, political, geographic, and family barriers also contribute to vaccine hesitancy.
Next, Groves highly recommended APhA’s
She noted that APhA suggests that pharmacists can help by having conversations with patients that begin with empathy. For example, the Playbook states, “Some people just need information and assurance. They may be anxious, uninformed, or misinformed. They need a safe space to voice their questions and concerns and get accurate information from a trusted source.”3 Groves told Drug Topics® that patients need to feel listened to and understood. She cited the recommend 3-step process from the Playbook when talking to patients about COVID-19 vaccines, but the system works just as well with other vaccinations.
The Playbook recommends the following process3:
- Elicit: APhA recommends asking patients what they already know, and what concerns they have that are causing them to hesitate. They recommend allowing the person to share without correcting or interrupting them.
- Provide: First pharmacists can ask the patient if they may share what they know, and then provide their knowledge in a nonjudgmental and neutral way. APhA recommends pharmacists avoid criticizing the person’s sources of information.
- Elicit: Pharmacists can then ask the person for their reaction to their explanation. Patients can be asked what they think of the information, or be asked “Where does this leave you now?” or “What else would you like to know?”3 “Continue with this Elicit–Provide–Elicit cycle until all of the person’s concerns are addressed,” the APhA suggests.3
When the cycles are complete, pharmacists can offer a strong, evidence-based recommendation and wrap up the conversation hopefully with vaccination on the spot or an appointment, APhA advised.3 Unfortunately, about 20% of people are not convinced by evidence-based explanations due to confirmation bias and other factors.3 One study found that when people reject evidence-based information the reasons are because of high levels of reactance (such as being nonconformist), having conspiratorial worldviews, and having strong disgust reactions to blood and needles.3 APhA also listed conformity bias as an issue, when the behavior of groups of other people cause individuals to make similar decisions.
Groves said one of the most important things that pharmacists can do to encourage vaccination is make that strong recommendation to the patient. “As pharmacists, we are recognized as trusted members of the patient’s care team. Assure patients that you are confident in vaccines to protect them and their families. The support pharmacists offer and the prebuilt trust patients have from being cared for by their pharmacists hopefully transfers to completed vaccinations. It’s the relationship between pharmacists and patients that is key to fighting vaccine hesitancy,” Groves said.
References
- Vaccine hesitancy: A growing challenge for immunization programmes. News release. World Health Organization (WHO). August 18, 2015.Accessed August 30, 2022.
https://www.who.int/news/item/18-08-2015-vaccine-hesitancy-a-growing-challenge-for-immunization-programmes - Larson HJ, Gakidou E, Murray CJL. The vaccine-vesitant moment. N Engl J Med. 2022;387(1):58-65. doi:10.1056/NEJMra2106441
- How to talk to people about COVID-19 vaccines. American Pharmacists Association. Accessed August 30, 2022.
https://vaccineconfident.pharmacist.com/Learn/Vaccine-Confident-Playbook/How-to-Talk-to-People-About-COVID-19-Vaccines
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.