Considerations for Atopic Dermatitis in Skin of Color
Skin of color can require different treatment options for atopic dermatitis.
In her RAD virtual conference presentation, Z. Pressley Rice, MD, FAAD, dermatologist at Dermatology Associates of Georgia in Atlanta, Georgia focused on the differences and disparities of atopic dermatitis (AD) in patients of skin of color (SoC), or pigmented skin that includes individuals from a variety of races and ethnic groups.
She emphasized the challenges of dermatological diseases in SoC:
-few studies have investigated Soc differences in epidemiology of dermatologic diseases
-little focus on SoC in medical school and residencies, creating low awareness that can impact diagnosis
-healthcare discrepancies affecting patients with SoC
-delayed treatment courses
-increased morbidity, ranging from melanoma and non-melanoma skin cancer to chronic inflammatory diseases
-shortage of participant diversity in clinical trials and lack of peer-reviewed literature on SoC
Numerous studies show that AD places a major burden on the SoC population. Evidence suggests that AD has a higher prevalence in some SoC populations than in Caucasians.
African Americans are 3 times more likely to be diagnosed with the condition than Caucasians, and Asian and Pacific Islanders are 7 times more likely to be diagnosed with it as compared to White counterparts.
There is also research to suggest AD has a greater quality of life impact in SoC patients, including:
-African Americans typically have more doctor visits for AD than Caucasians.
-non-Hispanic black and non-Hispanic children are more likely to have persistent AD than non-Hispanic White children.
-AD may be less controlled among African Americans versus White patients.
Rice said the reasons for the disparities could be biologically based (genetics) or socioeconomic. African American patients are at a higher risk of transepidermal water loss, causing dry skin, which has been studied in multiple small trials. This greater risk of dry skin would be consistent with a higher prevalence of AD. Rice noted that this could stem from socioeconomic causes, as opposed to biological. It could also be caused by genetic variations like the Filaggrin null mutations that could contribute to skin barrier dysfunction. Different racial populations have unique variations of FLG mutations.
Earlier studies show a detection of various immune axis markers in SoC AD patients, such as Th17/22 involvement in some Asian patients. Price noted that these findings may or may not generally hold for other Asian or African American populations. In addition, it is unknown whether AD pathogenesis itself differs in these patients exhibiting such markers because of the small cohorts.
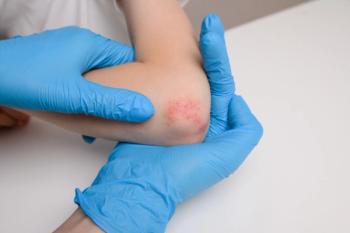
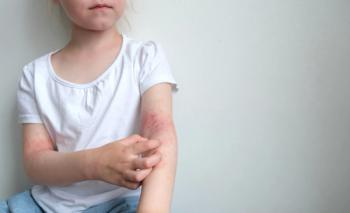
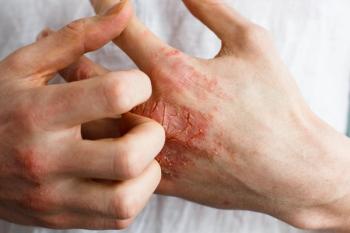
Rice said there is an underestimation of AD severity in SoC. Erythema may be difficult to identify or appear differently in heavily pigmented skin and can present differently such as pink or violet. Edema, skin warmth, or scaling are all indications of underlying erythema. Rice noted that the masking of erythema may prevent early diagnosis of AD and lead to the development of more severe diseases.
While the general treatment options for AD are similar across ethnicities, there are some considerations for clinicians to understand. Proactive therapy with topical corticosteroid is the standard treatment for chronic inflammatory diseases like AD, but in darker skin types, long-term use can worsen hypopigmentation. Ultraviolet phototherapy is another common treatment, but the dosing and duration of treatment are all issues to be considered for patients of color.
Rice indicated throughout the presentation that as the population in the United States becomes more diverse, it is crucial for clinicians to familiarize themselves with the special circumstances of treating AD in patients with SoC, and that additional data on the efficacy of common therapies for SoC are needed as well.
This article originally appeared on Dermatology Times.
Reference
Pressley-Rice, Z. The shades of atopic dermatitis in skin of color. RAD 2022 Conference; December 11, 2022.
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.