Chronic Inflammatory Skin Diseases and Shingles Risk
Study suggests higher hospitalization rate for some skin diseases.
Identified
A new study published in the
The study’s authors—Raj Chovatiya, MD, PhD, and Jonathan I. Silverberg, MD, PhD—analyzed data from the 2002 to 2012 Nationwide Inpatient Sample, which provides a representative cohort of hospitalizations in the United States. They concluded that hospitalization for shingles was significantly associated with several CISDs, including atopic dermatitis (AD), and that there was a greater length of stay for those patients
“Nearly one in three people in the US will develop herpes zoster in their lifetime, with approximately 1 million cases annually and a 3% hospitalization rate,” the authors wrote in the study. “Patients with chronic inflammatory skin diseases have potential risk factors for HZ, including long-term use of systematic immunosuppressants and immune dysregulation in the skin and periphery.”
The authors also reported that HZ hospitalization was associated with the female sex and extensive use of corticosteroids, and inversely associated with an increased number of chronic conditions and early adult age. They concluded that additional studies are needed to establish CISD-specific vaccination guidelines, particularly for individuals who are younger than the age recommended for HZ vaccination.
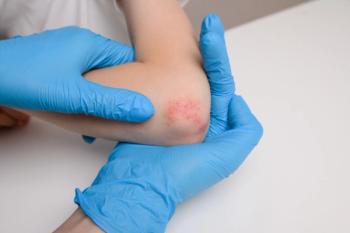
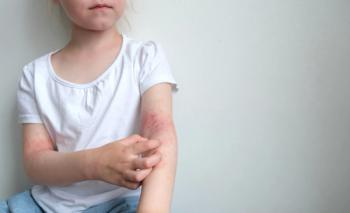
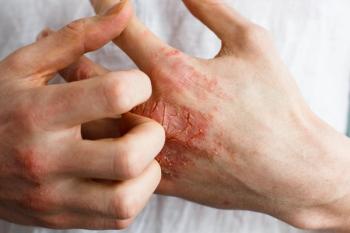
AD is the most common, chronic, and severe type of eczema, a non-contagious group of dermatologic conditions that cause red, irritated, itchy and/or inflamed skin. Statistics from the
In its earliest stages,
Two other important differences that set the shingles rash apart from other rashes are that shingles is typically much more painful, and it clears up within a few weeks. By comparison, eczema is a chronic condition that can stretch from childhood to adulthood.
Since the distribution of
Shingrix’s efficacy in preventing shingles has been reported to be as high as 97% in individuals 70 and older, and its efficacy for the prevention of the shingles complication
Reference
Chovatiya R, Silverberg JI. Association of herpes zoster and chronic inflammatory skin disease in US inpatients. Journal of the American Academy of Dermatology. 2020. Doi:
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.