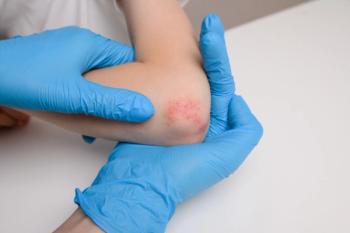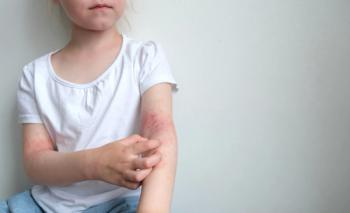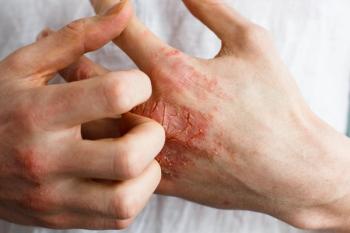
Atopic Dermatitis Patients See Decline in HRQOL Since Pandemic's Start
Certain problems related to health-related quality of life (HRQOL) became more common among patients with atopic dermatitis since the start of the COVID-19 pandemic.
Patients with atopic dermatitis (AD) reported more problems related to symptoms and quality of life during the COVID-19 pandemic, according to multiple measurement tools. The findings were
Researchers evaluated four measurement tools: the EuroQol-5 Dimension 5-level version (EQ-5D-5L), Skindex-16, Dermatology Life Quality Index (DLQI) and DLQI Index-Relevant (DLQI-R), a recently proposed scoring formula of the DLQI for avoiding possible bias in the “not relevant” response option. In addition to testing the measurement properties of these measures in adults with AD using a cross-sectional survey, they compared health-related quality of life (HRQOL) in these patients before and since the start of the pandemic.
The cross-sectional survey was carried out in Hungary and involved 2 academic dermatology clinics. Data was collected from March 2018 to March 11, 2020 (before COVID-19) and June 2020 to January 2021 (since COVID-19). Patients completed EQ-5D-5L, DLQI/DLQI-R, Skindex-16, a 0- to 10-item assessment for self-reported severity and questions about the history of their disease as well as their sociodemographic information. Dermatologists completed a second section with clinical information the Investigator Global Assessment (IGA), Eczema Area and Severity Index (EASI) and objective SCORing Atopic Dermatitis (oSCORAD).
A total of 218 patients completed the questionnaire. The mean age was 31.3 years and the majority (57.8%) were women. Thirty-five patients had dermatologic comorbidities and 194 had nondermatologic condition(s). According to the responses, 9.6% of patients were untreated, 63.3% were on systemic (nonbiologic) therapy, 23.4% were on topical therapy, 2.3% were on biological therapy and 1.4% were receiving phototherapy.
EASI identified 22.1% of patients having severe AD compared with 45.6% with oSCORAD, and 21.2% according to IGA. Severity scores did not differ significantly before and since COVID-19. While there were no significant differences in total HRQOL scores before and since COVID-19, more patents reported problems in specific areas.
Since COVID-19, more patients reported pain/discomfort (73.1% vs 60.0%) and anxiety/depression (55.9% vs 49.6%) on the EQ-5D-5L. On the DLQI, more patients reported problems with shopping/home/garden (82.8% vs 53.6%) and working/studying (72.8% vs 64.8%) since COVID-19. On Skindex-16, more patients reported problems with hurting (84.9% vs 75.6%), persistence/recurrence of AD (98.9% vs 91.9%), worry (97.8% vs 92.7%) and interactions with others (80.0% vs 72.8%) since COVID-19.
According to the authors, patients who had more severe disease had worse HRQOL across all outcome measures. However, they noted that patients with AD in the sample had quite severe overall HRQOL impairment both before and during the pandemic with a relatively high average DLQI even among the patients who had clear or mild AD.
“Based on our study, Skindex-16, DLQI, and DLQI-R also have good convergent and known-group validity in AD that make them appropriate instruments for HRQOL assessment in both clinical and research settings,” they noted.
One of the limitations was that given where they recruited from, the patients with moderate and severe AD may have been overrepresented compared with patients with mild AD. Another limitation was that AD-specific questionnaires could not be used because they do not have a Hungarian version.
Given the strong performance of EQ-5D-5L, DLQI, DLQI-R and Skindex-16 against validity tests, the authors suggested they “may be used as standalone measures or to complement AD-specific HRQOL instruments in clinical trials and daily practice.”
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.