What’s New With Continuous Glucose Monitors
Continuous glucose monitors are poised to change diabetes management for patients.
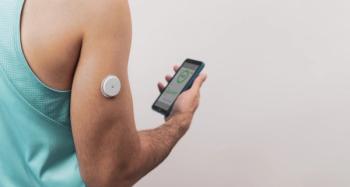
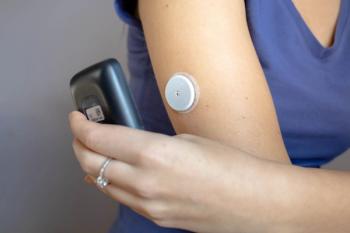
Continuous glucose monitoring devices (CGMs) have transformed the way diabetes is managed, pharmacists tell Drug Topics, and exciting new technology promises to further help patients with the disease.
“CGMs used to be limited for only certain patients but are now more widespread. The availability and affordability of these items have led to a large increase in their use, with many now being available at local pharmacies,” Kevin Fuschetto, PharmD, BCACP, assistant professor of Pharmacy Practice at Northeast Ohio Medical University in Rootstown, Ohio, and director of clinical services for NEOvations Pharmacy Services, LLC in Rootstown.
CGM technology is rapidly changing and improving, Fuschetto noted. One newer product is Abbott’s FreeStyle Libre 3 system. “This CGM system has improved on the prior Libre sensors, by decreasing the size (now about the size of 2 stacked pennies) and becoming a real-time CGM system, which means the patient does not have to do anything to see their glucose readings,” he said. Earlier Libre CGMs models required the patient to “scan” their sensor to see their glucose reading, according to Fuschetto.
Dexcom has also released a new CGM system, the Dexcom G7. The device combines the CGM sensor and transmitter into 1 disposable device that is “60% smaller, has a shorter warm-up period and has an approval for use in pregnancy, including gestational diabetes,” Fuschetto explained.
In addition to the Dexcom G7 and the Freestyle Libre 3, other popular CGMs include Medtronic’s The Guardian, the Dexcom G6, the Freestyle Libre 2 and Libre 3, and Ascencia’s Eversense E3, according to Diana Isaacs, PharmD, BCPS, endocrine clininical pharmacy specialist and director of education and training in diabetes technology at Cleveland Clinic Endocrinology & Metabolism Institute in Cleveland, Ohio.
“There are unique features of each [CGM], and pharmacists can help advise on the features and what may be an optimal choice per the individual,” Isaacs told Drug Topics. "For example, certain devices can integrate with specific connected insulin pens and insulin pumps. There are differences in costs, size of the CGM, and compatibility with smartphones and receivers.”
CGMs that are connected directly with certain insulin pumps and connected insulin pens “help simplify the care for patients using insulin pumps,” Fuschetto said. Sensor-augmented pumps use the data from the CGM to determine the amount of insulin to be delivered based off real-time glucose readings, which helps to lower the risk of hypoglycemia and limit hyperglycemia in patients, according to Fuschetto.
“I am also excited about the new and improved technology including insulin pumps with CGM that would avoid the need to bolus and become more like a true artificial pancreas,” Isaacs said. For example, Medtronic has been studying closed loop systems that would remove the need for boluses, she noted.
Although CGMs are helpful, they can easily be overwhelming for patients, Fuschetto said. “Many patients have heard of CGMs but may not understand the difference between a reading from a traditional fingerstick glucose and a reading from a CGM. Often, patients are given prescriptions for CGMs but have not been taught how to place and start a new sensor. These are all areas pharmacists are trained and skilled to advise their patients on.”
Pharmacists can advise patients on setting optimal alarms and alerts for use, how to share data, and how to understand data, Isaacs noted. For example, pharmacists can explain the meaning of time in range (the time spent between 70 mg/dL and 180mg/dL) and what the time in range goal is, which is over 70% for most people with diabetes.
“Pharmacists can empower people with diabetes to learn from their data and see the direct effects of foods, physical activity and medications to engage in positive health behaviors,” Isaacs added.
Professors at Northeast Ohio Medical University believe it is important for future students to “understand, interpret, and help manage diabetes technology, such as CGMS, insulin pumps, and connected insulin pens,” Fuschetto said. "We realize this is a growing aspect of diabetes management and one pharmacists should be trained and prepared to be experts on.”
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.