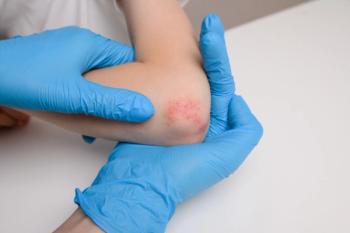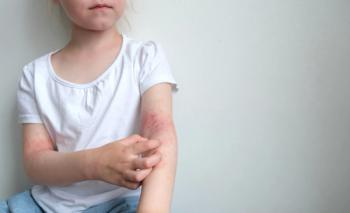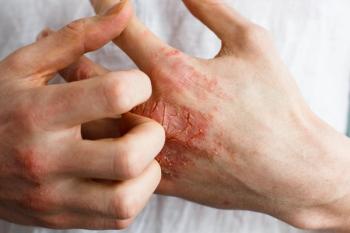
Simplifying Widespread Itch Care with Targeted Solutions
Matthew Zirwas, MD, shares his step-by-step pearls for quelling the pruritic skin condition.
Effective management of frequently debilitating itch starts with understanding type.Matthew J. Zirwas, MD, offered tips for diagnosing and treating widespread itch with little to no rash as part of his presentation at the recent New Wave Dermatology Conference.1
“Itch is an interesting space,” Zirwas told Dermatology Times®. “It gets more and more complicated the more we know about the mechanism but simpler and simpler in terms of managing itch. There are some really helpful things that most people in dermatology just aren’t aware of that I love teaching about.”
Zirwas, an associate professor at Ohio University Heritage College of Medicine in Athens, Ohio, covered new research on itch and practical recommendations for translating that to patient care.What followsare his tips for addressing the unique characteristics of widespread itch that does not present with an obvious rash.
Diagnosis Details
Zirwas noted there is “no identifiable cause in the vast majority of [these] cases.” When there is, “it is usually a diagnosis that predated the start of the itch. It is in the medical history, not something you’re going to diagnose because of the itch.”
For cases with itch that “is all over, all the time,” he advised first “considering and usually ordering” these tests: complete blood count, comprehensive medical panel, thyrotropinhemoglobin, and hemoglobin A1c. “If merited by the individual case, I would consider, but rarely order, hepatitis B and C, HIV, , and a chest x-ray.”
However, in some patients with persistent, widespread itch, it may be necessary to weigh whether to test for cancer, he added. “The only overrepresented [types] are bile duct malignancy and hematologic malignancy,” he said, and both are typically going to be detected with routine labs (leukemia, hypereosinophilic syndrome, etc with a CBC) or exam (bile duct malignancy because of jaundice, as the itch starts after the bile duct is blocked, lymphoma via lymph node exam).“So, order age-appropriate malignancy screens, do a lymph node exam, conduct a complete review of symptoms, and work up any abnormals aggressively.” However, he cautioned, “Don’t go fishing if the review of systems, physical exam and basic labs are normal.”
Treatment Strategies
Steroids remain a standard first-line treatment for widespread itch, although studies suggest that their role in itch reduction may be more attributable to their action in improving the skin disease overall by decreasing inflammation rather than by directly reducing itch.2
“If a systemic steroid doesn’t work, it suggests the itch is not immunologic/inflammatory,” Zirwas said. “If it does work, the itch could still be neuropathic as steroids work on everything.”
For generalized itch, Zirwas said it is “reasonable” to give patients a 3-week steroid taper to show improvement. “If they do [improve], find the minimum dose to relieve itch and use it chronically,” he said. A prednisone equivalent of 10mg should be prescribed every other day or less, he noted, , as at this dose (5 mg/d or less of prednisone) the risk of short or long term side effects from systemic steroids is quite low, even with long term use
Although he has both male and female patients who have responded to this dosing regimen for prednisone without major adverseeffects, it is not the right choice for every patient. “If prednisone works but the necessary dose it too high, something like methotrexate is worth a trial.” The starting point could be 5 mg to 10mg weekly, which, said Zirwas, “increases the activity of regulatory Tcells so it isn’t suppressing the immune system—it’s balancing it.”He finds low dose methotrexate particularly useful in elderly patients, in whom he suspecta the cause of itch is often unregulated, non-specific, sub-clinical inflammation related to an age related waning of Treg function.
Dexamethasone is another option. “I’ve found that 0.75 or 0.5mg can be used 10 days on and 4 days off. The 0.75 mg dose equals the anti-inflammatory efficacy of 25 mg of prednisone with the [adverse] effects of 5 mg,” Zirwas said.
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.