Shingles Vaccine Protects More Than Just the Recipient
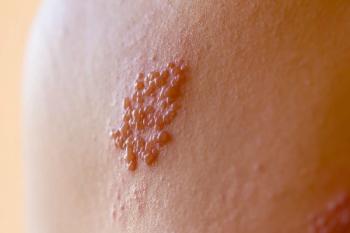
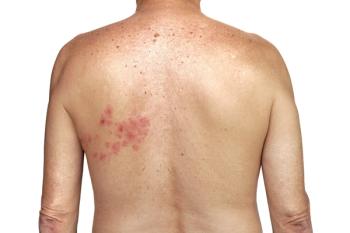
Herpes zoster exposure puts unvaccinated individuals at risk for chickenpox.
Most of the advice received by eligible recipients of the recombinant herpes zoster (HZ) vaccine (
Both chickenpox (varicella) and shingles, or HZ, are caused by the varicella zoster virus (
Although shingles itself is
Today, there are 2 effective chickenpox vaccines licensed for use in the United States, varicella virus vaccine live (Varivax) and measles, mumps, rubella and varicella virus vaccine live (ProQuad). The
However, millions of children, adolescents, and adults who have never had chickenpox or been vaccinated are at risk. Young children who have received only the first of 2 doses of vaccine recommended by the CDC are also susceptible.
A recent
“Chickenpox and shingles vaccines are both highly effective, so why is the latter only available to older adults?” Sarah Szczypinski wrote in the article. “How many young adults get shingles in the first place, and does the FDA age recommendation for the Shingrix vaccine prevent them from getting it? And most importantly, do parents realize that unvaccinated kids—either because they are too young or by parental choice—might be at risk for chickenpox if they’re exposed to a shingles rash?”2
Adding to the conundrum is a recent study revealing that shingles is
The good news is that the
Another positive is that Shingrix, the vaccine approved for use in the US by the FDA in 2017 for people 50 years and older, is up to 90% effective at preventing shingles. Fewer cases of shingles means fewer potential infections that could lead to cases of chickenpox in at-risk children and adults.
References
1. Chickenpox Vaccination: What Everyone Should Know. CDC. Last updated August 7, 2019. Accessed December 2, 2020. https://www.cdc.gov/vaccines/vpd/varicella/public/index.html#:~:text=CDC%20recommends%20two%20doses%20of,age%204%20through%206%20years.
2. Szczypinski S. Rising Shingles Cases in Adults Put Unvaccinated Children at Risk. The New York Times. Published September 3, 2020. Last Updated September 7, 2020. Accessed December 2, 2020. https://www.nytimes.com/2020/09/03/parenting/chickenpox-shingles-vaccine.html
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.