Shingles Vaccination Counseling During the COVID-19 Pandemic
CDC advises not to delay shingles vaccination.
New
In general, the health organization noted that efforts to reduce transmission of the COVID virus through stay-at-home and shelter-in-place orders have resulted in a decreased use of routine preventive medical services, including immunization.
“Ensuring that routine vaccination is maintained or reinitiated during the COVID-19 pandemic is essential for protecting individuals and communities from vaccine-preventable diseases and outbreaks,” the CDC stated in the
Webinar:
Specific to shingles vaccination, the CDC encourages health care providers to administer both doses of Shingrix to eligible patients within the recommended interval of 2 to 6 months. If more than 6 months elapse between the first and second doses, the second dose should be administered as soon as possible.2
Counseling about potential
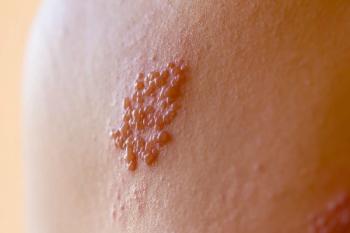
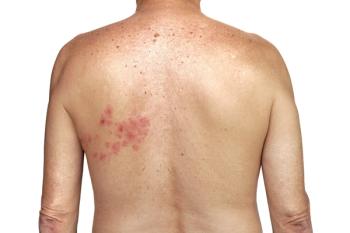
Typical AEs associated with Shingrix include local reactions like redness, pain, and swelling at the injection site, as well as systemic reactions like fever, chills, headache, and body aches. All of these reactions normally resolve within 72 hours after vaccination.
As a result of concerns related to COVID-19, the CDC advised that patients who develop fever after vaccination should stay home until they have been fever-free for 24 hours without the use of fever-reducing medications.2
Additionally, it’s important to note that Shingrix does not cause the respiratory symptoms associated with COVID-19. “If a vaccine recipient develops symptoms of COVID-19 (eg, cough or shortness of breath), or if fever does not resolve within 72 hours of vaccination without the use of fever-reducing medications, the recipient should contact their health care provider,” advises the CDC. “If a vaccine recipient develops emergency warning signs for COVID-19, emergency medical care should be sought immediately.”2
The CDC also asks health care providers to defer vaccination for patients with suspected or confirmed COVID-19, regardless of symptoms, until they have met the
“Health care personnel, whether they administer vaccines or not, should take steps to ensure that their patients continue to receive vaccines according to the
References
1. CDC. Frequently asked questions about Shingrix. Last updated October 5, 2020. Accessed March 1, 2021.
2. CDC. Interim guidance for routine and influenza immunization services during the COVID-19 pandemic. Last updated October 20, 2020. Accessed March 1, 2021.
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.