Shingles and Menopause: Is There a Connection?
The link between menopause and shingles may be explained by hormones, stress, and immunity.
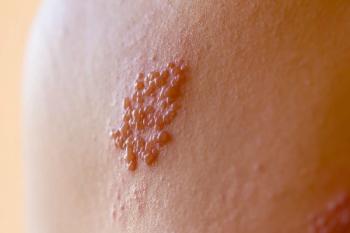
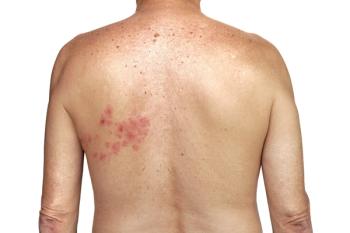
Shifting hormones, hot flashes, mood swings, sleep deprivation, and short-term memory loss are all normal and natural changes women experience and anticipate during menopause. However, many women may be unaware that they are also at an increased risk for developing shingles (herpes zoster) while transitioning through menopause.
Herpes zoster (HZ) is a reactivation of the
The menopause/shingles connection generally focuses on three factors: hormones, stress, and immunity.
According to the North American Menopause Society (
In her OBGYN practice in Ithaca, NY, Kathleen Gardner, MD, witnesses first-hand how hormones, stress, and immunity interact in her menopausal patients. “Herpes zoster is a reactivation of a virus that looks for opportunities of physiologic stress, and menopause is a time of both physiologic and emotional stress,” she said.
For example, hormonal disruptions associated with menopause affect sleep patterns. “Poor sleep patterns clearly play a role in overall health, but also play a role in immunologic health,” added Gardner.
NAMS Past President Marla Shapiro, CM, MDCM, points out that while there are gender differences when it comes to shingles, conclusive research data is lacking when it comes to shingles and women per se. “We often jump to the conclusion that these gender differences must be hormonal because it’s happening in 50 and 60 year olds, but we really don’t know if there are pathophysiological causes in gender differences,” she explains. “There are a number of theories that look at the fact that estrogen and progesterone may tamp down the inflammation, so in their absence during the onset of menopause we could lose that protection. But a lot of it is quite theoretical.”
NAMS advocates for the best protection against preventable diseases. The shingles vaccine is among the most valuable vaccinations for midlife women, according to NAMS.
Shapiro offered specific guidance to all women as well as men. “When you hit age 50, you really want to think about getting the shingles vaccine,” she said. “For those who had the attenuated live virus vaccine [Zostavax], we’re still recommending reimmunization with 2 doses of the recombinant vaccine [Shingrix].” She noted that
Effective July 2020,
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.