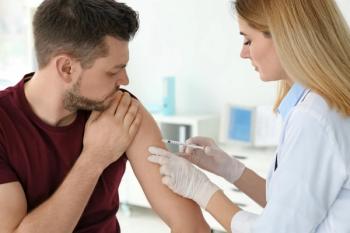
HPV Vaccine Rates Rise in Teens When They Can Consent, Research Shows
State legislation that allows adolescents to choose to receive the HPV vaccine without parental interference would elevate immunization rates, according to a new study.
Policies allowing teens to consent to human papillomavirus (HPV) vaccination may be a key strategy in improving vaccine uptake in adolescent populations, according to a research report published in JAMA Pediatrics.
The HPV vaccine is important in preventing disease and has proven safety and efficacy. Despite this, data reveal only 54% of adolescents in the United States are vaccinated with the complete HPV vaccine series.
Researchers evaluated the link between consent for the HPV vaccine and vaccination rate. Using data from a national dataset, investigators broke adolescents up into 2 categories based on whether they were or were not able to consent to vaccination.
The study cohort included data from 81,899 teenagers, collected between 2015 and 2018 from the states that allow adolescent consent to vaccination, including Alabama, Alaska, California, Delaware, Idaho, New York, Oregon, and South Carolina, as well as Washington, DC. Participants were aged 13 to 17 years (mean age, 15±1.4 years) and 49% were girls.
Those who received the first dose of the series of HPV vaccine doses was in states that allowed adolescent consent, 67.9% of adolescents began the HPV vaccine series, vs 61.4% among adolescents who were not able to consent due to state laws. Completion of all 3 HPV vaccination doses was 53.7% among adolescents, compared with 47.9% who could not consent.
In the sensitivity analysis, vaccine series initiation was significantly associated with the ability to consent. According to researchers, this analysis “revealed a significant positive association between adolescent being permitted to consent to HPV vaccination by state laws in their location of residence and increased rates of initiation of the vaccine series.”
Study limitations include the “cross-sectional nature” of the analyses, which prevented the researchers from establishing causality.
“This suggests that policies that permit adolescents to consent to HPV vaccination could be an important strategy toward improving vaccine initiation among young adolescents, when the vaccine is most likely to be effective,” the researchers concluded.
Reference
1. Ashlynn R. Torres BA. State Laws Permitting Adolescent Consent to Human Papillomavirus Vaccination and Rates of Immunization. JAMA Pediatrics. Accessed November 19, 2021.