An Abundance of Options for Treating Atopic Dermatitis
Across the globe, new drugs — injections, topical and oral — are being developed to help patients with atopic dermatitis.
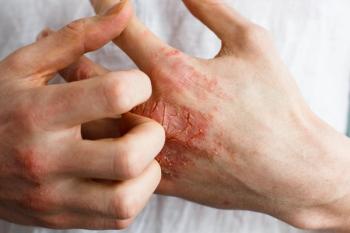
Atopic dermatitis, also known as eczema, is a chronic inflammatory skin condition affecting up to 10% of adults and 20% of children in the United States. It is characterized by persistent severe itching and skin barrier disruptions. The cycle of itching and scratching perpetuates inflammation and damage to the skin, leading to infections and diminished quality of life. Symptoms of AD can disrupt sleep and have negative social and emotional effects.
Until recently, treatment for atopic dermatitis has been limited to topical corticosteroids and calcineurin inhibitors for mild to moderate AD, whereas systemic steroids, immunosuppressants and phototherapy were used for moderate to severe cases. The systemic treatments are effective but come with undesirable side effects.
An overactive immune response under the skin and compromised skin tissue on the surface are the source of AD symptoms. New agents target immune system pathways and cells directly involved in the pathology of the condition.
Janus Kinase Inhibitors
Researchers have shown that AD may be partially caused by overactivity of Janus kinases (JAKs), a group of inflammatory cytokines. The JAKs include JAK1, JAK2, JAK3 and tyrosine kinase 2. Blocking JAK signaling pathways can dampen the production of cytokines responsible for AD symptoms, and inhibiting select JAKs can help manage specific AD symptoms.
New JAK inhibitors have been used for several autoimmune diseases, and a handful are moving through the pipeline as potential treatments for AD. The JAK inhibitors are an important addition to AD treatment for people who haven’t responded to other treatments.
“They’re amazing for these (patients with more severe cases). They have a huge, huge impact on quality of life,” said Peter A. Lio, M.D., at a session on atopic dermatitis at the annual meeting of the Academy of Managed Care Pharmacy in March. Lio is a clinical assistant professor of dermatology and pediatrics at Northwestern University’s Feinberg School of Medicine and founding director of the Chicago Integrative Eczema Center.
Incyte’s Opzelura (ruxolitinib) cream is the first topical JAK inhibitor approved by the FDA as a treatment for AD. Opzelura, which received approval in September 2021, is a JAK1 and JAK2 inhibitor indicated for the short-term treatment of mild to moderate AD in patients age 12 and older.
Earlier this year, the agency approved two oral JAK1 inhibitors that address the need for systemic therapy for moderate to severe AD. Pfizer’s Cibinqo (abrocitinib) promises relief for adults with refractory moderate to severe AD and AbbVie’s Rinvoq (upadacitinib) was approved as a treatment for adults and children age 12 and older with refractory moderate to severe AD.
Olumiant (baricitinib), an oral JAK1 and JAK2 inhibitor comarketed by Eli Lilly and Incyte, was the first of its class approved in the European Union and Japan to treat moderate to severe AD in adults. In phase 3 studies, once-daily dosing of Olumiant, combined with topical corticosteroids, significantly improved signs and symptoms of AD compared with placebo and topical corticosteroids. The companies say they are on track to complete an additional phase 3 study later and are awaiting approval from the FDA.
Delgocitinib, a topical JAK inhibitor, inhibits all members of the JAK family. It is approved in Japan as a topical ointment for adults and children age 2 and older. The drug was developed by Japan Tobacco and is distributed under the brand name Corectim by Torii Pharmaceutical, a Japanese company.
Danish company Leo Pharma is conducting phase 3 trials investigating the potential use of a delgocitinib cream in adults with moderate to severe chronic hand eczema, a type of atopic dermatitis affecting the fingers and back of the hands.
Further back in the topical JAK inhibitor pipeline is a product being developed by Aclaris Therapeutics. After failing to meet end points with its first investigational topical JAK inhibitor, Aclaris is following up with topical solution ATI-1777. This JAK1 and JAK3 inhibitor showed positive results in a phase 2a trial, and the company has said it will move forward with a larger phase 2b trial for potential use in adults with AD.
Monoclonal Antibodies
Monoclonal antibodies play a significant role in alleviating AD symptoms through blockage of cytokines critical to AD pathophysiology. The cytokines interleukin (IL)-4, IL-13 and IL-31 are of particular interest. AD’s skin barrier disruptions are driven by inhibition of certain proteins essential for healthy skin barrier function. IL-4 and IL-13 play a significant role in inhibiting those proteins. IL-31 promotes activation of the itch response on nerve cells and eosinophils, a type of disease-fighting white blood cell.
In 2017 the FDA approved Dupixent (dupilumab), an IL-4 receptor antagonist developed by Regeneron and Sanofi, to treat AD in adults. Lio sees Dupixent as a turning point in AD treatment: “It has changed everything and allows us to really offer sustained control for a huge group of people who never had it before, in a really safe way,” he said at the AMCP meeting.
In May 2020 the FDA approved Dupixent for children age 6 and older, and in August 2021 the companies reported meeting all end points in a phase 3 trial evaluating the use of the monoclonal antibody in children as young as 6 months. Adbry (tralokinumab), developed by Leo Pharma, is an IL-13 antagonist approved by the FDA in December 2021. Both biologics offer systemic treatment for moderate to severe atopic dermatitis not responding to topical treatments.
In August 2021, the FDA gave Lilly’s IL-13 inhibitor, lebrikizumab, a fast track designation, which means more frequent meetings with the FDA and a rolling review, both of which are intended to shorten the time to an approval decision.
Nemolizumab, an IL-31 inhibitor from Swiss dermatology specialist Galderma, is another drug in late-stage development. By binding to IL-31 receptors, nemolizumab keeps the interleukin from potentiating the itch sensation. In phase 2 studies, there was significant reduction in itching in patients taking nemolizumab compared with those taking placebo.
Tapinarof
Tapinarof is a topical first-in-class therapeutic aryl hydrocarbon receptor-modulating agent developed by biopharmaceutical company Dermavant Sciences. It is a nonsteroidal topical option for patients with mild AD. Tapinarof inhibits pathways involved with inflammatory cytokines that mediate AD symptoms. After positive phase 2 trial results, Dermavant started a phase 3 trial evaluating the use of tapinarof cream in patients age 2 and older with AD.
Difamilast
New Jersey-based Medimetriks and Japan’s Otsuka Pharmaceuticals are developing difamilast, a topical phosphodiesterase-4 (PDE-4) inhibitor for patients age 15 and older with mild to moderate AD. PDE-4 is involved in the production of proinflammatory cytokines responsible for symptoms of AD and other inflammatory disorders. In two phase 3 trials conducted in Japan, a higher proportion of patients who received difamilast ointment experienced clear to almost-clear skin compared with participants who used placebo. Otsuka announced in September 2021 that Japanese regulators had approved difamilast, which in Japan is being sold under the brand name Moizerto. Medimetriks is preparing to launch phase 3 trials in the U.S. If difamilast makes it on to the market, it would join Eucrisa (crisaborole) as the second topical PDE-4 inhibitor used for AD treatment. The FDA approved Eucrisa in 2016.