US Shingles Update: Cases Up, but Vaccination Rates Increasing
Decades after the introduction of the chickenpox vaccine and 14 years after the first shingles vaccine was approved in the United States, it’s time to take stock of where the country is in respect to shingles infections
Decades after the introduction of the chickenpox vaccine and 14 years after the first shingles vaccine was approved in the United States, it’s time to take stock of where the country is in respect to shingles infections. The bad news is infection rates are up; the good news is there is an effective shingles vaccine that holds promise for the future.
First, some background on the subject from Jeffrey I. Cohen, MD, chief, Laboratory of Infectious Diseases at the National Institutes of Health (NIH). Shingles (herpes zoster, or HZ) is caused by a reactivation of the varicella zoster virus (
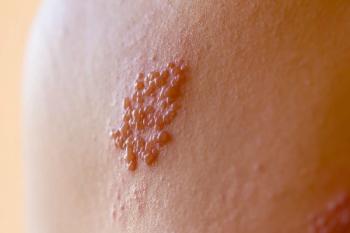
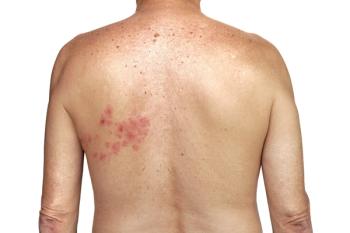
This is the scenario that plays out for approximately 1 in 3 Americans, accounting for an estimated 1 million cases of shingles annually. According to the
One study reported on by
The reasons for the overall rise in rates are unclear. Prior to the introduction of the varicella vaccine in 1996, there was speculation in the medical community that the number of shingles cases would increase based on the theory that exposure to chickenpox boosts an individual’s immunity to VZV and reduces the risk that it will reactivate as shingles. That is, as more children received the varicella vaccine and the number of chickenpox cases declined, shingles cases in adults would rise.2
However, 2 subsequent CDC studies found that the shingles rates began increasing in the US before the chickenpox vaccine was introduced and did not increase faster afterwards. Additionally, there have been similar increases in shingles rates in countries that do not have routine chickenpox vaccination programs.2
One important question remains unanswered: Will shingles eventually just disappear once generations of people have been vaccinated against chickenpox? “Epidemiologists are predicting that it will go away, or at least become very rare in the US,” said neurologist Anne Louise Oaklander, MD, PhD, and director of the Nerve Unit at Massachusetts General Hospital. “We hope that with the new vaccination this will become of historical interest only. But it’s very much with us right now.”
Recent data from the CDC revealed that the
Shingrix is now the only shingles vaccine since Merck
References
1. CDC. Shingles (Herpes Zoster). Page last reviewed: August 14, 2019. Accessed September 3, 2020.
2. What Are Trends in Emergency Department Utilization, Costs for Shingles? News Release. JAMA Dermatology; June 21, 2017. Accessed September 3, 2020.
Newsletter
Pharmacy practice is always changing. Stay ahead of the curve with the Drug Topics newsletter and get the latest drug information, industry trends, and patient care tips.